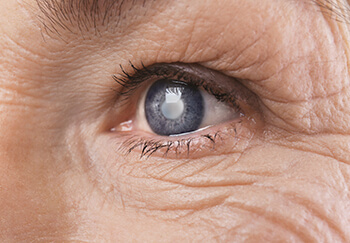
A cataract is the clouding of the lens inside the eye, causing blurry or hazy vision and sensitivity to glaring light. There has never been a better time to have cataract surgery because of all the vision improvement options available. To our patients throughout the Birmingham area, once you have decided to have cataract surgery you and your doctor will work together to decide what type of artificial intraocular lens (IOL) is right for you.
Cataract Surgeon at VisionFirst Eye Center
How do I know if I have a cataract?
A cataract is the result of a natural change inside your eye making your vision less sharp over time. Usually, cataracts form with age, but can also be caused by trauma, disease and family history. Your eye doctor will check for the presence of cataracts. The examination is important because it demonstrates what effects cataracts may be having on your visual acuity. It’s also possible that the cataract may not warrant medical treatment. Sometimes changing your glasses prescription may help.
Cataracts develop slowly and painlessly and you may not realize your vision is changing. Symptoms of cataracts include the following:
- Blurred vision
- Poor night vision
- Faded color vision
- Double vision
- Sensitivity to light
For patients with glaucoma or ocular hypertension, VisionFirst Eye Center is participating in the Spyglass Pharma Clinical Study.
What is Astigmatism?
Cornea shape differs from person to person and astigmatism is very common. Astigmatism occurs when the cornea or windshield of the eye is not perfectly round. A common description is that a cornea with astigmatism is shaped more like a football than a basketball. Astigmatism causes blurry vision that can be corrected with glasses, contact lenses, refractive surgery, or at the time of cataract surgery.
If you wear toric contact lenses or glasses full time, you have astigmatism correction that you may or may not be aware of. Astigmatism matters at the time of cataract surgery because people who have astigmatism but select basic lens technology should expect to wear glasses or toric contacts lenses full time after surgery for clear vision.
What is Cataract Surgery?
Cataract surgery involves removal of the cataract or cloudy lens and insertion of a new, clear, prosthetic lens implant which is typically made of acrylic or silicone material. A small incision is made on the surface of the eye, the lens capsule is opened, and an ultrasound probe is used to break up and remove your cataract.
The intraocular lens is then folded and injected inside the eye. Most commonly the lens capsule that held your natural lens holds the artificial lens implant. In almost all cases, an artificial lens implant must be placed after your cataract is removed for you to see without an extremely thick pair of glasses. These lens implants are well tolerated and last a lifetime in most cases. The surgery itself takes approximately 20-30 minutes and is performed in a sterile operating room using mild sedation. You will not be completely asleep during surgery. You should expect to be at a surgery center for several hours for pre-operative and post-operative care.
Your Cataract Treatment Options
When determining which cataract package interests you, decide if you are willing to wear glasses full-time, part-time, or as little as possible. This will help guide your selection.
When deciding about investing in surgical and lens technology remember to consider the additional cost of glasses, prescription sunglasses, and/or contact lenses during your lifetime. These expenses are often significantly larger than the one-time cost of surgery using premium technology. In general, cataract surgery is covered by your insurance. This includes use of the operating room, anesthesia, and equipment for surgery.
However, reducing your dependence on eyeglasses is not considered medically necessary. As a result, your insurance will cover a basic lens implant but no other lens technologies.
Basic Cataract Surgery –
$0 Per Eye
Basic cataract surgery is just as it sounds. The lens implant is covered by your insurance but does not offer any range of vision without glasses. The goal of basic surgery is to improve your vision with glasses. Pre-operative testing will be minimal to include only what insurance will cover. Glasses and/or contact lenses are often required full-time after basic cataract surgery.
The $0 per eye for the lens implant does not mean you will have no out-of-pocket expense for your surgery. It means that you will not be paying extra for the artificial lens implant that is placed in your eye during cataract surgery
Advanced Cataract Surgery – $2200 Per Eye
Advanced cataract surgery provides a Toric intraocular lens for correction of astigmatism (defocus). This is a good option for people who want clear distance vision with the use of reading glasses only or for people who have astigmatism but want blended vision with a distance target in one eye and an intermediate or near target in the other eye. Premium measurements and pre-operative analysis prior to surgery to best select the appropriate lens technology is included in this price.
It is important to follow our Step 2 instructions regarding use of preservative-free tears and warm compresses beginning 2 weeks prior to your appointment in order to ensure the most accurate measurements for this technology.
Premium Cataract Surgery – $3100 Per Eye
Premium cataract surgery involves use of an extended depth of focus, multifocal, or trifocal intraocular lens implant that not only corrects astigmatism, but provides for a broader, more natural range of vision without glasses.
Premium measurements and pre-operative analysis prior to surgery to best select the appropriate lens technology is included in this price. It is important to follow our Step 2 instructions regarding use of preservative-free tears and warm compresses beginning 2 weeks prior to your appointment in order to ensure the most accurate measurements for this technology.
Prepare for your surgery by learning more about the Cataract surgery procedure.








